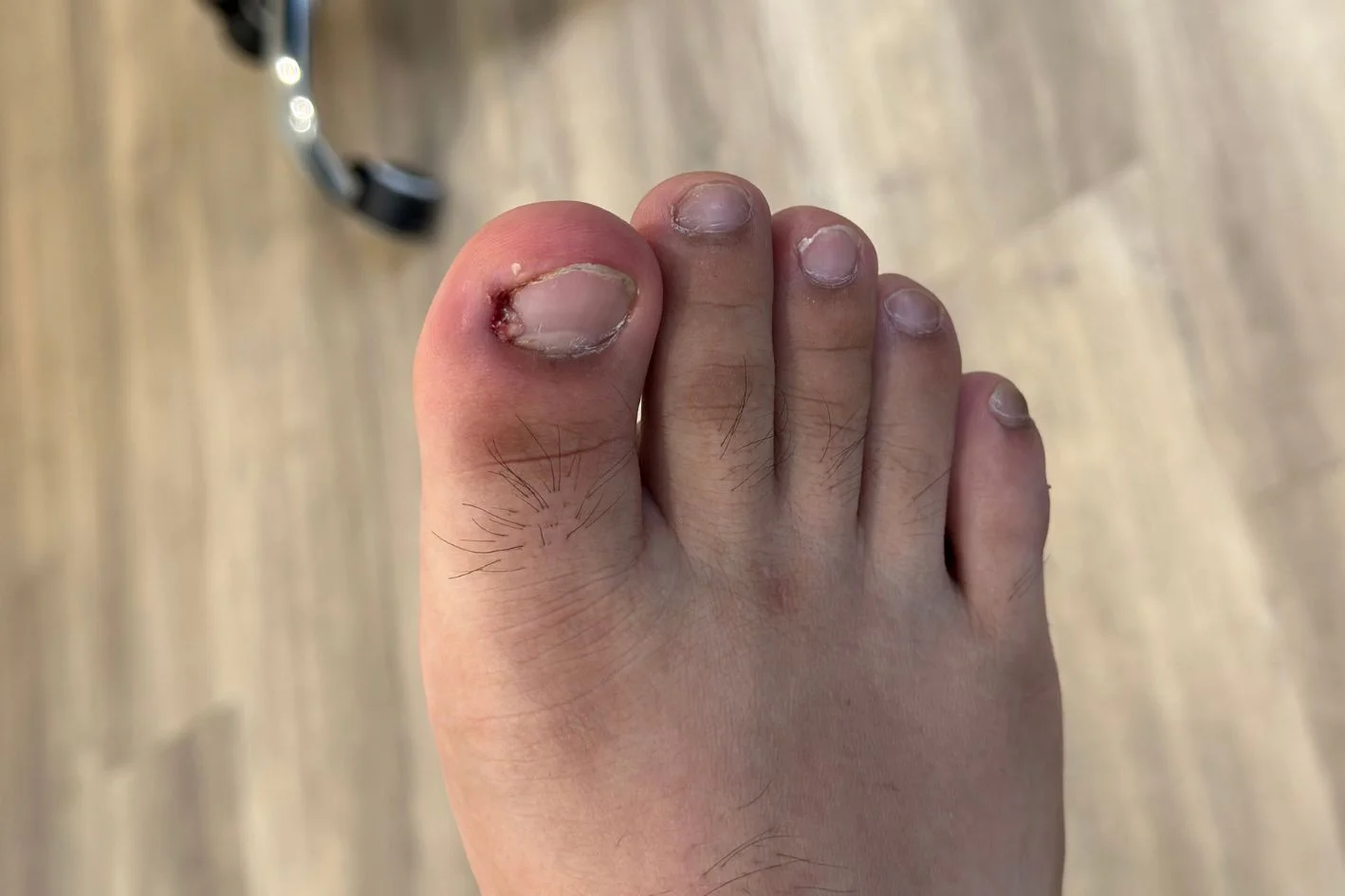
Both conditions cause pain at the nail fold, both make footwear feel unbearable, and both frequently appear at exactly the same time in exactly the same toe. The overlap is close enough that patients, and sometimes general practitioners too, regularly treat one while missing the other. Understanding the distinction matters not because the two conditions are entirely unrelated, but because they have different primary drivers, and treating the infection without addressing the nail, or managing the nail without clearing the infection, tends to produce results that do not hold.
The same nail fold anatomy is involved in both. The nail fold is the strip of skin that runs alongside and behind the nail plate on three sides. It is a site that receives repeated mechanical pressure from footwear, experiences limited airflow, and is regularly exposed to moisture in Singapore’s climate. When that tissue is in trouble, the symptoms often cluster together: redness, swelling, tenderness when the toe is pressed, and sometimes pus. The pattern within those symptoms is what separates the two conditions, and it is worth looking at each individually before comparing them directly.
What an Ingrown Toenail Is Doing to the Tissue
An ingrown toenail is a mechanical problem. The nail edge, typically the corner of the big toenail, has grown or been cut in a way that causes it to press into the adjacent nail fold rather than sitting cleanly above it. The nail is not infected. It is physically breaching soft tissue that is not designed to bear a sharp edge.
The body responds to this mechanical intrusion the way it responds to any foreign object embedding in soft tissue: with inflammation. The nail fold becomes red, swollen, and tender, and as the nail continues to grow forward, it carves a small wound channel into the tissue. Hypergranulation tissue, a type of raised, fleshy new tissue, often forms at the wound site. This is the body attempting to wall off the intrusion. The process happens gradually, often over weeks, and patients frequently recall a shift in how they cut the nail or a period of wearing tighter footwear shortly before symptoms began.
The key clinical feature of an ingrown toenail is that you can identify the nail edge as the source. Press along the side of the nail where the edge meets the fold, and a sharp, poking pain maps precisely to that point. The offending edge may not be visible as it is embedded into the tissue, but it is typically palpable beneath the swollen fold. The problem is structural: remove the mechanical pressure, and the tissue irritation has a chance to resolve. This is why open-toed footwear and rest provide real, immediate relief for ingrown toenails, and why the pain returns as soon as an enclosed shoe compresses the fold back against the nail edge.
What Paronychia Is Doing to the Tissue
Paronychia is an infection of the periungual tissue, the soft tissue directly surrounding the nail plate. The primary problem is microbial, not mechanical. Bacteria or fungi have entered the nail fold through a break in the skin barrier, and the redness, swelling, warmth, and pain are the body’s immune response to organisms establishing themselves in the tissue.
The immediate distinguishing feature is the degree of warmth. In an early stage of an uninfected ingrown toenail, the tissue is tender and inflamed from mechanical trauma. In paronychia, the tissue is warm, as with infected tissue: noticeably hotter to the touch than the surrounding skin and often throbbing without any direct pressure applied. This is the increase in blood flow driven by active infection, not just localised irritation from a nail edge.
Pus is a reliable indicator of paronychia when it is present. A small pocket of cream or yellow-white fluid beneath the skin surface near the nail fold is not something an ingrown toenail produces on its own. When pus appears, bacteria have established a contained colony in the tissue. This is unlikely to resolve without either spontaneous drainage or clinical intervention.
Acute paronychia develops quickly, often within a day or two, with symptoms escalating noticeably over that window. Chronic paronychia develops gradually over weeks, tends to cause a gradual loss of the cuticle, and may produce subtle nail plate changes, such as ridging or surface irregularities, as sustained inflammation near the nail root disrupts normal nail growth.

Need Help? See A Podiatrist Today
Where the Two Conditions Overlap
The confusion between these two conditions is not a mistake on the patient’s part. Ingrown toenails cause paronychia. When a nail edge creates a persistent wound in the nail fold, it gives bacteria a direct, reliable entry point into tissue that is warm, moist, and not well-ventilated. The wound does not need to be large. A nail edge pressing into the fold applies enough repeated tissue damage to compromise the skin barrier, and from there an infection has an accessible route in.
This means many patients presenting with paronychia are also managing an ingrown toenail without realising the two are connected. The infection is the visible, painful problem. The nail edge is the mechanism sustaining it.
The combined presentation can look like this: sharp pain along the nail edge with visible redness and swelling, discharge or pus near the nail corner, warmth extending slightly beyond the immediate wound site, and a nail edge that is partially embedded in or clearly pressing against the swollen fold. The tissue does not always separate cleanly into “the nail problem” and “the infection problem” when both are present simultaneously.
What Happens When You Treat Only One
Where an ingrown toenail is driving repeated bouts of paronychia, treating only the infection produces short-term improvement but not a lasting resolution. The antimicrobial treatment reduces the bacterial load and the acute inflammation settles, but the nail edge remains in place. The wound channel is still there. The next time the toe is compressed in footwear, or the nail grows forward slightly, the conditions for a new infection are re-established. This is precisely the type of cases we see in our clinics almost everyday: Patients who are caught in the pattern of going through repeated courses of antibiotics for a toe infection without the nail ever being reviewed.
The reverse matters too. Where someone has an ingrown toenail managed conservatively, by cutting back the nail edge, but there is already an established paronychia, the infection needs to be addressed alongside or before the nail work. Manipulating an acutely infected nail fold without managing the infection can drive the bacterial process deeper into the tissue or cause unnecessary pain during the procedure.
How to Tell Them Apart at Home
No single feature is definitively diagnostic without a clinical examination, but the following patterns help separate the two:
- If the pain maps precisely to the nail edge where it presses against the fold, and that is the only area of significant tenderness, an ingrown toenail is likely the primary driver
- If the tissue is noticeably hot to the touch, throbbing without contact, or producing pus beneath the skin, an infection is present regardless of what originally caused it
- If symptoms developed gradually over weeks and are linked to footwear changes or a recent nail cut, an ingrown toenail origin is more probable
- If symptoms appeared over hours to a day or two with escalating warmth and swelling, acute paronychia is the more likely primary problem
- If you have had multiple episodes of the same toe becoming inflamed and settling with antibiotics, only to flare again weeks later, an ingrown nail driving repeated infections is the most common explanation
As podiatrists, a useful question you can ask yourself is whether you can feel or see a nail edge pressing into the fold. If the corner of the nail is buried in or pressed against the swollen tissue, the structural problem needs to be addressed, not just the infection sitting on top of it.
When to Get a Clinical Assessment
Self-managing with warm soaks and careful nail hygiene is reasonable for a very mild, early presentation. Once pus has formed beneath the skin, the infection is unlikely to clear without drainage. Once an ingrown toenail has created a persistent wound channel, conservative nail care alone does not resolve the structural driver.
A partial nail avulsion removes the nail edge that is causing the mechanical injury, addressing the source of repeated infections and allowing the nail fold tissue to heal without the ongoing pressure that has been sustaining the problem. For straightforward paronychia without a structural nail component, the management focus shifts to an antimicrobial approach and to protecting the periungual barrier as it heals.
If the toe has been painful for more than a week, if pus is present, if the redness is spreading beyond the immediate nail fold, or if the same toe keeps becoming infected after treatment, seeing a podiatrist will give you a clearer picture of what is driving the presentation and what will actually resolve it rather than manage it temporarily.