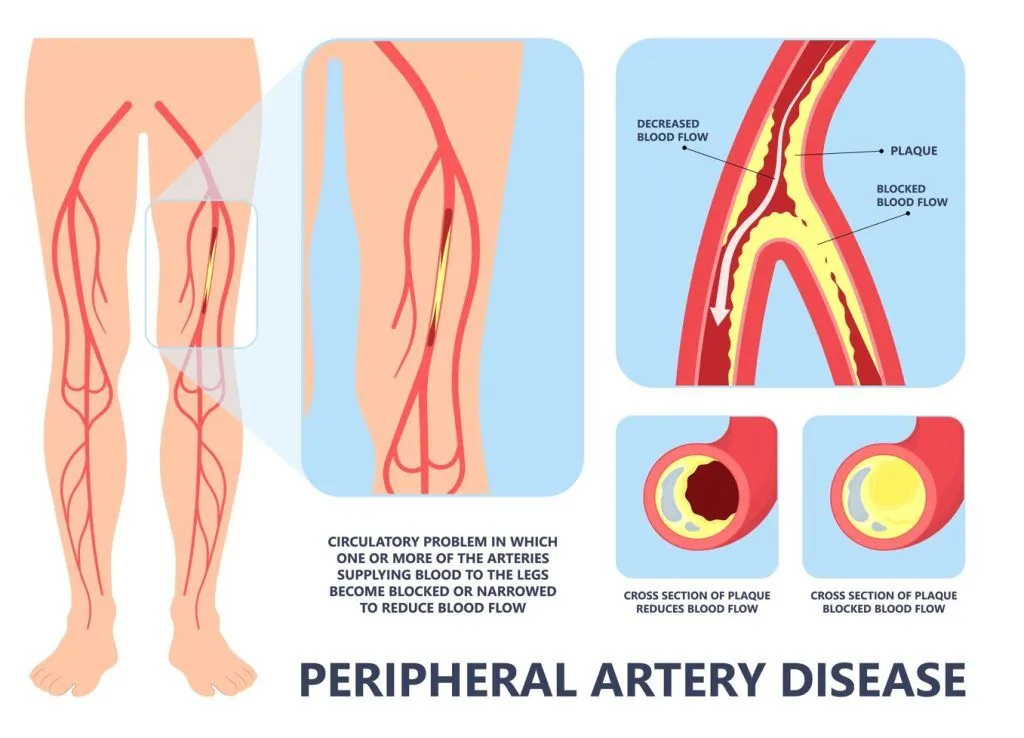
What is Peripheral Arterial Disease?
周围动脉疾病 (PAD) 是一种常见且严重的疾病,会影响心脏和大脑以外的动脉或血管,导致血流减少或阻塞。下肢(腿和脚)最常受到影响,并可能导致截肢。
People with diabetes have a higher risk of developing PAD because the high blood sugar levels damage blood vessels and impair blood flow. As a result, people with diabetes must manage their condition effectively and be vigilant about potential PAD symptoms.
外周动脉疾病的症状
外周动脉疾病的症状可能包括:
- 腿部疼痛或抽筋(尤其是在进行体育活动时),
- 麻木或无力
- 下肢发冷
- 皮肤颜色变化(皮肤暗沉且呈紫色)
- 难以愈合的伤口或溃疡。
如果您出现上述任何症状,或有糖尿病病史,应咨询足病医生或医疗专业人员以进行进一步检查。
外周动脉疾病的诊断
要诊断外周动脉疾病(PAD),我们需要进行全面检查,具体包括以下内容:
- 检查脉搏
- 检查双腿和双脚,查看是否有外周动脉疾病(PAD)的迹象。
- 临床诊断检查,如踝肱指数、多普勒超声
如果怀疑患有外周动脉疾病(PAD),您的医生可能会建议您进行进一步的影像学检查,例如CT血管造影和磁共振血管造影。
治疗与管理
The treatment for PAD varies depending on the severity of the condition, which the imaging scans can determine. Restoring blood flow is urgently needed if there is the presence of a non-healing wound or when the patient is in severe pain.
Treatment options for PAD in Singapore include:
- Lifestyle Changes: Healthy habits can improve PAD symptoms and slow progression. Quit smoking, exercise regularly, and maintain a balanced diet.
- Controlling Your Sugar Levels: You should maintain healthy blood sugar levels. If you have diabetes, you must regularly check with your doctor to monitor your condition.
- Medications: Your doctor may prescribe medications to control blood sugar, blood pressure, and cholesterol levels. Additionally, they may recommend medications to prevent blood clots and alleviate pain associated with PAD.
- Surgical and Nonsurgical Procedures: In more advanced cases, procedures like angioplasty, stenting, atherectomy, or bypass surgery by a vascular surgeon may be necessary to restore blood flow and relieve symptoms.
PAD on Wound Healing
Peripheral Arterial disease can significantly impact wound healing, particularly in people with diabetes. When blood flow to the extremities is reduced or blocked, it leads to impaired delivery of oxygen and essential nutrients, resulting in slower wound healing and an increased risk of infection.
PAD’s Impact on Wounds:
- Delayed Healing: Due to reduced blood flow, wounds may take longer to heal, increasing the likelihood of complications such as infections.
- Increased Risk of Infection: Reduced blood flow makes wounds more susceptible to bacterial infections, further delaying healing and increasing the risk of serious complications.
- Gangrene and Amputation: In severe cases of PAD, blood flow to tissues can be so limited that it leads to tissue death or gangrene. If the gangrene becomes extensive beyond treatable, amputation of the affected limb may be necessary.
Managing Wounds with PAD
Wounds with underlying PAD, especially diabetic foot wounds, should be handled with adequate care to prevent serious complications. Your podiatrist or healthcare professional should help you with the following:
- Appropriate Wound Care: Proper wound care promotes healing in individuals with PAD. Wounds must stay clean, dry, and covered with dressings prescribed by your podiatrist or healthcare professional.
- Offloading Pressure: High pressure stops wounds from healing. Your podiatrist will typically prescribe specialized footwear, cushions, or orthotic devices to help redistribute the pressure.
- Infection Control: Be vigilant about any signs of infection, such as increased pain, redness, swelling, or foul-smelling discharge. If you suspect an infection, seek medical help immediately.
- Vascular Treatment: Addressing the underlying vascular issues is crucial for promoting wound healing. Your podiatrist should work closely with a vascular surgeon to develop your treatment plan.
- Regular Check-ups: A regular weekly review of your wound is necessary. Regular reviews allow podiatrists or medical professionals to intervene promptly if complications arise.
把这个分享给你认识的人
Frequently Asked Questions on Peripheral Arterial Disease
When should I seek medical attention for PAD?
You should seek medical attention for peripheral arterial disease (PAD) if you experience any related symptoms or signs, especially if you have diabetes, high blood pressure, high cholesterol, or smoking history. Related symptoms of PAD include:
- Persistent leg pain or cramping, especially when walking or doing physical activity
- Numbness, weakness, or tingling in the legs or feet
- Frequent leg cramps or burning pain at night
- Coldness, colour changes, or shiny skin on the legs or feet
- Non-healing leg or foot wound for more than two weeks
How can I prevent PAD complications?
You should maintain a balanced diet and aim for at least 150 minutes of moderate-intensity exercise. If you have diabetes, you should also closely monitor your blood sugar levels, take your medications as prescribed, and have regular follow-up reviews with your doctor. Lastly, check your feet daily for any skin breaks or appearance changes. You should seek medication immediately if you notice any unusual skin changes.
Can peripheral arterial disease recur if I had undergone treatment before?
Unfortunately, PAD can potentially recur. If you have a history of PAD, you must monitor your condition and have regular reviews with your podiatrist or healthcare professional. Prompt medical attention can help you prevent complications such as tissue damage, infection, or amputation.
What types of wounds are most commonly associated with PAD?
Wounds most commonly associated with PAD are leg and foot arterial ulcers, particularly in individuals with diabetes. These ulcers result from reduced arterial blood flow and, if left untreated, can lead to tissue death or amputations.
Gangrene is the end-stage of PAD, where the reduction in blood flow causes tissue to die extensively. Gangrene typically begins from the toes. If the PAD remains untreated, it will progressively spread towards the foot and ankle.
What kind of follow-up care and long-term management can I expect after PAD treatment in Singapore?
Your medical professional will guide you on follow-up care, which generally includes regular check-ups, blood tests, and imaging studies to monitor your condition. Long-term management usually involves lifestyle modifications, medication adjustments, and ongoing collaboration with your healthcare team to address all underlying risk factors and prevent complications.